Listen to the article
WASHINGTON — Popular GLP-1 weight-loss medications have helped millions of people shed pounds, but new research from Australia suggests doctors and patients may need to pay closer attention to what users are actually eating while taking them.
A systematic review from the Hunter Medical Research Institute (HMRI) found that while the medications are effective for weight loss, many clinical trials fail to track changes in diet or whether patients are still getting enough essential nutrients. According to researchers, that gap could increase the risk of malnutrition over time.
“Very little is known about the exact changes these medications have on what people actually eat, whether vitamin and mineral intakes are adequate, and whether weight-loss achieved through medication also supports optimal nutrition-related health and wellbeing in the long-term,” stated researchers from HMRI.
One concern highlighted in the review is the potential for vitamin deficiencies — including rare cases of scurvy, a disease caused by a lack of vitamin C. Historically known as “pirate’s disease,” scurvy develops when the body doesn’t receive enough fruits and vegetables to maintain healthy tissue repair and immune function.
Symptoms of scurvy can include anemia, loose teeth, bruising, bleeding under the skin, swollen or bleeding gums, and wounds that don’t heal. These symptoms can significantly impact quality of life and overall health if left unaddressed.
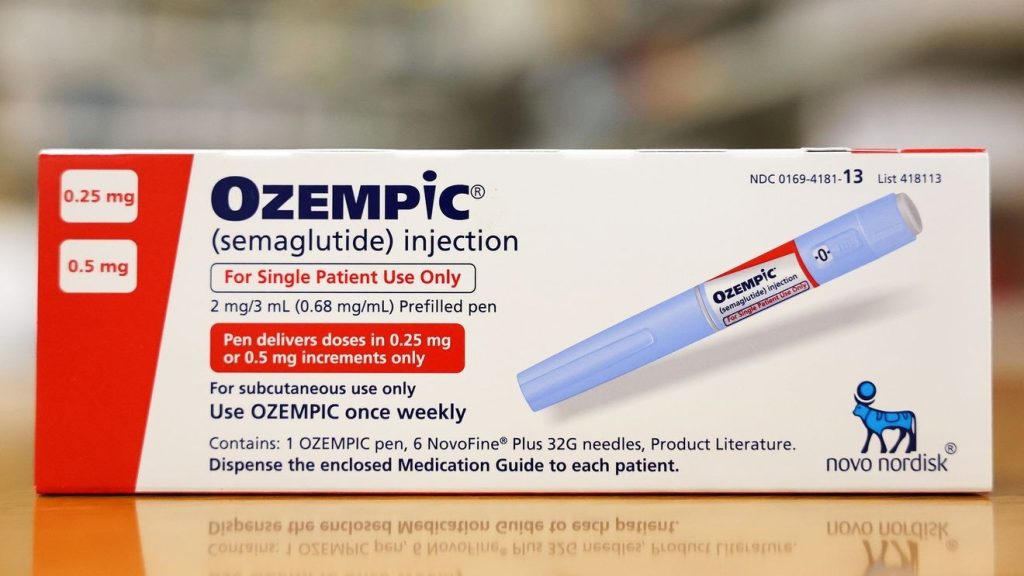
The rising popularity of GLP-1 medications, including brands like Ozempic, Wegovy, and Mounjaro, has transformed the weight loss landscape. Originally developed for type 2 diabetes, these drugs work by mimicking hormones that regulate appetite and blood sugar. Their effectiveness has led to widespread use, with some patients reporting significant weight loss of 15% or more of their total body weight.
However, the rapid reduction in food intake that accompanies these medications may have unintended consequences. Beyond vitamin C, researchers say other deficiencies could also pose risks. Iron deficiency can lead to anemia, while low levels of certain B vitamins may contribute to serious neurological conditions such as Wernicke’s encephalopathy — though experts note these complications remain rare.
Dr. Jessica Bartfield, an obesity medicine specialist not involved in the research, explained in a recent interview that “these medications work primarily by slowing gastric emptying and increasing feelings of fullness. This means patients naturally eat less, but it also means they need to be more intentional about food quality.”
Another challenge, researchers say, is that symptoms of nutrient deficiency — including fatigue, nausea, and irritability — can overlap with the common side effects of GLP-1 medications, making problems harder to spot early. This overlap can lead to delays in identifying and addressing nutritional issues.
Experts stress that these cases appear uncommon and that the findings are not a call for people to stop taking GLP-1 medications. Instead, the results point to a major blind spot in current research that needs to be addressed through more comprehensive clinical studies.
Doctors are now being urged to monitor patients’ diets more closely and ensure that even smaller meals remain nutritionally dense. The review also calls for future clinical trials to include detailed dietary assessments to better understand long-term health effects.
The global market for GLP-1 medications is expected to reach $100 billion by 2030, according to industry analysts. This explosive growth underscores the importance of understanding the full impact of these drugs on patients’ nutritional health.
For patients concerned about their nutritional status, experts recommend working with a registered dietitian and considering screening for deficiencies before starting treatment. Simple blood tests can identify potential vitamin and mineral deficiencies, allowing for early intervention.
“The key is not to avoid these medications, which have proven benefits for many patients with obesity, but to use them as part of a comprehensive approach to health that includes nutritional awareness,” said nutritionist Sarah Hallberg, who specializes in medical weight management.
The bottom line from researchers: GLP-1 medications can be highly effective for weight loss, but long-term success depends not just on appetite suppression — it also requires careful nutrition management to avoid potentially serious deficiencies.
Fact Checker
Verify the accuracy of this article using The Disinformation Commission analysis and real-time sources.



11 Comments
The historical link between scurvy and pirates makes this research particularly intriguing. I wonder if certain populations or demographics are more susceptible to vitamin deficiencies with these weight-loss drugs. Nuanced monitoring seems warranted.
Yes, the pirate connection is quite fascinating. Further research into potential high-risk groups could help guide more targeted monitoring and dietary guidance for GLP-1 medication users.
This highlights the importance of holistic care when it comes to weight management medications. Focusing solely on the pounds lost misses critical nutritional considerations that can impact long-term health. A balanced approach is prudent.
The historical connection to pirate’s disease is a fascinating angle. I wonder if there are any other rare or overlooked nutritional issues that could emerge with widespread GLP-1 medication use. Vigilant monitoring seems prudent.
Scurvy may be a historical disease, but it’s a good reminder that radical dietary changes can have unexpected consequences. Careful management of GLP-1 medication use is prudent to avoid modern-day cases of this vitamin C deficiency.
Interesting research on the potential nutritional risks of GLP-1 medications. It’s important that doctors and patients closely monitor diet and nutrient intake to avoid deficiencies like scurvy during weight loss. Balanced nutrition is key for overall health.
Good point. Careful monitoring of nutrient intake is crucial to ensure these medications are used safely and effectively for long-term health.
This research raises important questions about the long-term effects of GLP-1 drugs on overall health and nutrition. While effective for weight loss, the potential for nutrient deficiencies is concerning and warrants closer examination.
Absolutely. The trade-offs between weight loss and nutritional status need to be better understood to ensure these medications are used safely and responsibly.
The finding that many clinical trials fail to track dietary changes and nutrient intake is concerning. Without that data, it’s difficult to fully understand the health implications of these weight-loss drugs. More comprehensive studies are needed.
I agree. Robust data on the nutritional impacts is essential for evaluating the risks and benefits of GLP-1 medications. Filling that research gap should be a priority.